How does Continuous Glucose Monitoring for Blood Sugar Tracking Work?
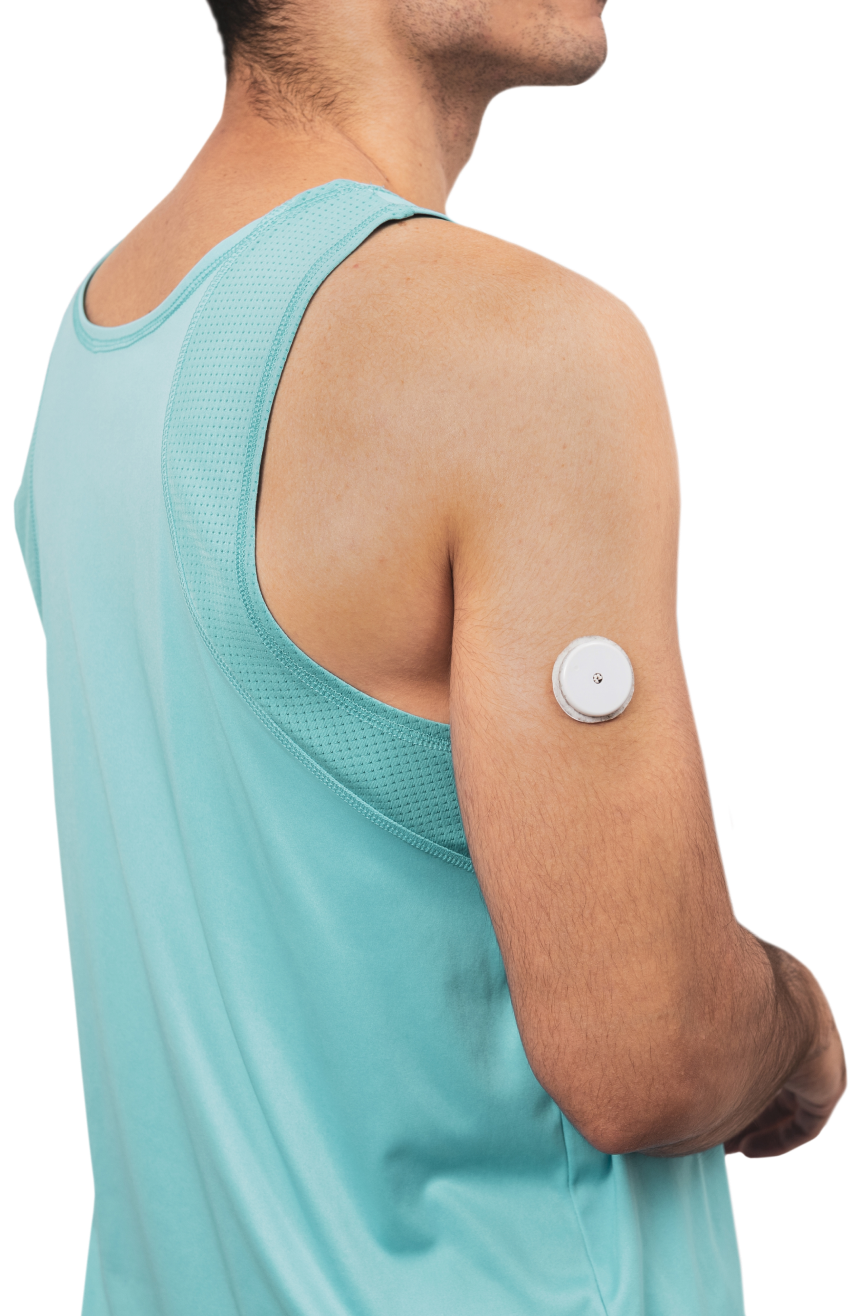
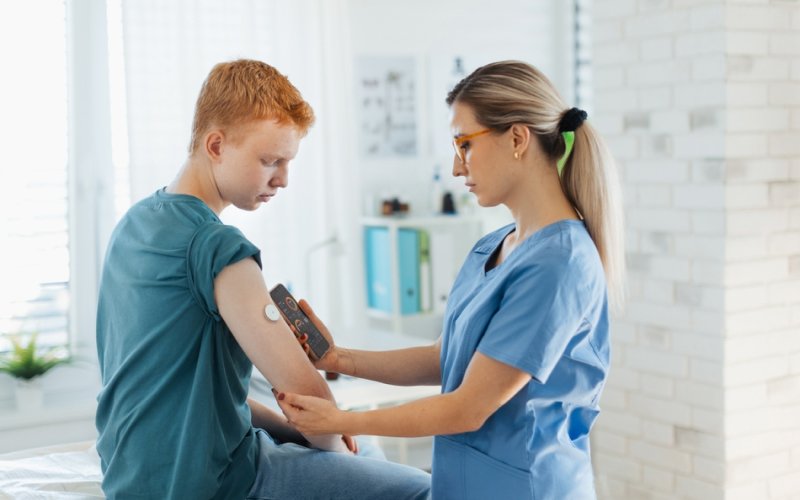
Continuous Glucose Monitoring (CGM) has revolutionized how we manage and track blood sugar levels. The device operates by inserting a tiny sensor under the skin which measures glucose in the tissue fluid. This data is then transmitted to a display device, allowing users to keep track of blood sugar levels in real-time. With CGM, individuals get a comprehensive view of their glucose trends, enabling better decisions on how to control blood sugar levels, ensuring they remain within a healthy range.